The Microbial Command Center
The gastrointestinal microbiota operates as a finely regulated biological system that extends its influence well beyond digestion. By producing short-chain fatty acids, it modulates enteric nervous system activity and directly affects intestinal barrier permeability, supporting overall systemic balance.
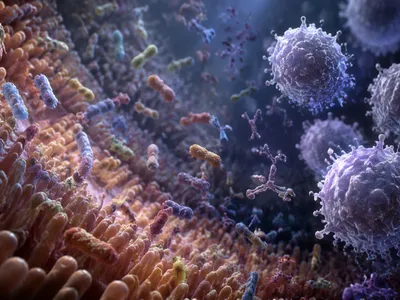
This microbial network also governs endocrine and immune functions by controlling serotonin-producing enterochromaffin cells and maintaining immune tolerance through gut-associated lymphoid tissue interactions. Acting as a core center for physiological integration, it is closely linked to metabolic, inflammatory, and neurological conditions when disrupted. Its function is further defined by a bidirectional communication loop with the host, allowing microbial metabolites to regulate gene expression in distant organs such as the liver and central nervous system.
Architects of Mood and Mind
Neural circuits governing emotion are profoundly shaped by microbial-derived signals, with tryptophan metabolism serving as a critical intersection between the gut and the brain.
Preclinical models reveal that germ-free animals exhibit exaggerated stress responses and altered social behaviors, deficits that are reversible through selective microbial reconstitution, highlighting the necessity of these organisms for normative affective processing.
Clinical investigations demonstrate that specific psychobiotic strains can reduce perceived stress and improve cognitive flexibility by modulating hypothalamic-pituitary-adrenal axis reactivity. These effects are mediated in part by vagal afferent neurons, which translate microbial metabolite profiles into central neurotransmitter release patterns, thereby influencing emotional salience and fear extinction learning. The therapeutic potential of targeting this axis is further emphasized by the ability of certain microbial interventions to alter functional connectivity in prefrontal-limbic circuits, offering a non-pharmacological avenue for managing mood disorders through precision microbial reconstitution strategies.
Metabolic Gatekeepers
Gut bacteria regulate energy harvest from dietary components and directly influence host metabolic pathways through a sophisticated array of bioactive compounds.
The conversion of dietary fiber into short-chain fatty acids such as acetate, propionate, and butyrate serves as a primary mechanism, activating intestinal gluconeogenesis and enhancing glucagon-like peptide-1 secretion to improve insulin sensitivity.
These microbial metabolites also modulate bile acid signaling via farnesoid X receptor pathways, affecting lipid absorption and cholesterol homeostasis. Disruption of this metabolic network is now recognized as a core feature of obesity, type 2 diabetes, and non-alcoholic fatty liver disease, where microbial diversity loss correlates with impaired glucose tolerance and chronic low-grade inflammation that perpetuates metabolic dysfunction across multiple organ systems.
| Microbial Metabolite | Primary Metabolic Function |
|---|---|
| Short-chain fatty acids | Enhance intestinal gluconeogenesis, increase GLP-1 and PYY secretion, reduce adipose tissue inflammation |
| Secondary bile acids | Activate FXR and TGR5 receptors, regulate lipid and glucose metabolism, modulate energy expenditure |
| Branched-chain amino acids | Contribute to insulin resistance when elevated; microbial balance influences circulating BCAA levels |
Fortifying the Body’s Barriers
Intestinal barrier integrity represents a critical frontier maintained by symbiotic bacteria through the regulation of tight junction proteins and the reinforcement of the mucosal layer.
Commensal organisms stimulate goblet cell differentiation and mucus secretion while simultaneously producing antimicrobial peptides that limit pathogen encroachment, thereby preventing the translocation of bacterial products into systemic circulation.
The tight junction complex, particularly occludin and claudin family members, is directly stabilized by microbial-derived butyrate through histone deacetylase inhibition. Loss of this microbial support results in increased intestinal permeability, or “leaky gut,” which has been mechanistically linked to the pathogenesis of inflammatory bowel disease, celiac disease, and even extra-intestinal conditions such as type 1 diabetes and multiple sclerosis where barrier dysfunction precedes clinical onset.
- 🧫 Reinforces mucus layer thickness via goblet cell stimulation
- 🔬 Upregulates tight junction protein expression through butyrate signaling
- 🛡️ Produces bacteriocins to suppress pathogenic bacterial overgrowth
- 🧪 Modulates secretory IgA production to maintain immune exclusion
The Gut-Immune Alliance
The intestinal microbiota maintains constant communication with the host immune system, guiding immune cells to differentiate between harmless antigens and harmful pathogens. Segmented filamentous bacteria promote Th17 cell accumulation in the lamina propria, enhancing defense against enteric infections while supporting immune regulation through Foxp3+ regulatory T cell induction.
Certain commensals, such as Bacteroides fragilis, actively limit inflammation by producing molecules like polysaccharide A that stimulate anti-inflammatory pathways. Colonization in early life is especially crucial, as it defines long-term immune responsiveness. Disruptions during this stage, described as dysbiosis during this period, are associated with increased susceptibility to allergies, asthma, and autoimmune diseases due to impaired immune tolerance.
Circadian Rhythms and Beyond
Gut microbial populations undergo daily fluctuations in composition and activity, closely aligned with host feeding rhythms through a reciprocal regulatory mechanism. Metabolites such as short-chain fatty acids and secondary bile acids regulate clock gene expression in intestinal and peripheral tissues, functioning as zeitgebers that help maintain circadian balance.
Feeding patterns, particularly time-restricted eating, can reshape the microbial environment by encouraging beneficial metabolite-producing bacteria while limiting those associated with metabolic dysfunction. This adaptive shift supports improved metabolic efficiency and overall host stability.
Conversely, circadian disruption caused by shift work or poor sleep promotes the growth of pro-inflammatory bacteria and reduces beneficial butyrate producers, weakening the intestinal barrier and increasing systemic inflammation. This dynamic interaction between circadian biology and microbiota highlights an emerging therapeutic approach, where aligning nutrition timing with microbial activity may help manage metabolic, inflammatory, and neurodegenerative disorders.